My Public Health Training
My Diagnosis
The Advanced Medical & Public Health Internship diagnosis is the first-ever program of its kind. I not only got to work with the top medical professionals from around the world, but I had the unique opportunity to learn about and practice patient examination, evaluation, and diagnosis.
Through virtual reality technology, I was connected with a clinic and maternity ward in Bauchi State, Nigeria where I was able to interact with my patients in real-time. Supervised by a doctor in Nigeria, I examined & diagnosed my patient using my diagnostic training on the top 4 leading causes of death in Nigeria; malaria, typhoid fever, nutritional anemia, & acute respiratory infections (ARI).
These patients were locals from Bauchi State that were all ill and would normally not be able to afford medical treatment as they earn $1.25 a day or less. In return for working with our participants, all of their treatments were funded by Leadership Initiatives.
In 2023, Leadership Initiatives was able to fund the treatment of all patients participating in this program.
My Public Health
Campaign
I learned about four of the most pertinent diseases in the developing world from medical professionals including Dr. Aisha Garba-Aliyu, medical doctor and public health expert in Nigeria.
With their guidance, I gained a better understanding of the signs and symptoms correlated with different stages and severities of malaria, typhoid fever, acute respiratory infections (ARIs), and nutritional anemia. I also developed cultural competencies and a global perspective to assess the structural and social determinants of health that underlie these diseases.
With the help of collaborating directly with development and public health experts to develop an impactful educational public health campaign. The campaign is specifically tailored to address the needs of underserved communities in Bauchi, aiming to raise awareness about ARIS and promote positive behavioral changes. Throughout the internship, I immersed myself in rigorous research and analysis to ensure the campaign’s effectiveness and relevance to the local population.
The process of creating the public health campaign was both challenging and rewarding. I conducted in-depth research on prevalent health concerns in the targeted communities, identifying key areas where intervention and awareness were essential for improving public health outcomes. Collaborating with mentors and fellow interns, I formulated innovative strategies to engage the community, ensuring the campaign’s messages would resonate with the intended audience.
Clinical Skills Training
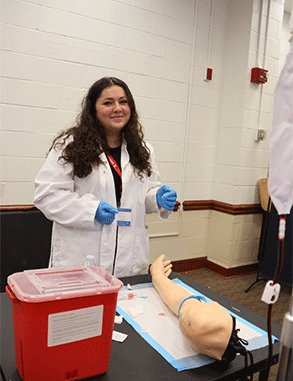
Phlebotomy
I learned how to draw blood using a phlebotomy arm simulator. Using this simulator allowed me to practice placing a needle in a vein to draw blood with realistic tissue-like material that imitates vein-wall resistance.
During this exercise, the medical facilitator instructed me on the proper technique and helped me improve the communication skills that I will use with future patients.

Laparoscopy
I learned about laparoscopy, which is a minimally invasive operation that allows physicians to observe and assess the abdomen or pelvis using small incisions and cameras. It is an invaluable tool for developing diagnoses and interventions.
Once I was familiarized with the function of this technology, I had the unique opportunity to apply this knowledge to perform a simulated laparoscopy.
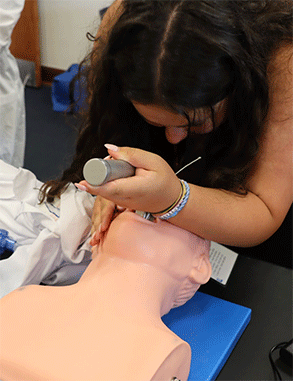
Intubation
I also worked with EMT instructors to learn how to perform multiple times of emergency resuscitation techniques including a manual esophageal intubation and a manual resuscitation airway mask.
The EMT helped me understand the proper situations to utilize different resuscitation and breathing assistance techniques and the proper equipment needed.
Internship Highlights
- Experts & Mentors
- Diagnostic Training
- Health Data
- CPR Certification
- Suturing & Casting

During this internship, I had the opportunity to learn from top medical professionals across various fields and specialties, including surgery, emergency medicine, and medical research.
Among these experts were Dr. Rachel Selekmen, a pediatric urologist and telehealth specialist, who shared insights into her career trajectory and a day in her life as a surgeon at Children’s National Hospital in DC. Additionally, Dr. James Giordano, Chief of Georgetown University’s Neuroethics Studies Program, provided valuable knowledge about his career and passion for neuroscience.
Through these interactions, I gained a comprehensive understanding of the responsibilities associated with each medical specialty and learned how to pursue these careers.

Under the mentorship of Dr. Garba-Aliyu, I learned essential skills in patient interviewing and disease investigation techniques. Throughout the program, I honed my abilities in collecting, interpreting, and critically analyzing patient data.
Dr. Garba-Aliyu’s guidance significantly enhanced my capacity to synthesize and evaluate information, crucial for the diagnostic process. These exercises allowed me to improve my communication skills for the effective evaluation of patients.
Dr. Garba-Aliyu’s expertise also provided me with a comprehensive understanding of current practices in Nigerian medicine. Meeting and learning from real patients allowed me to gain a deep appreciation for the lived experiences of individuals in Nigeria, influencing my perspective on implementing effective strategies in my campaign to combat infectious diseases.
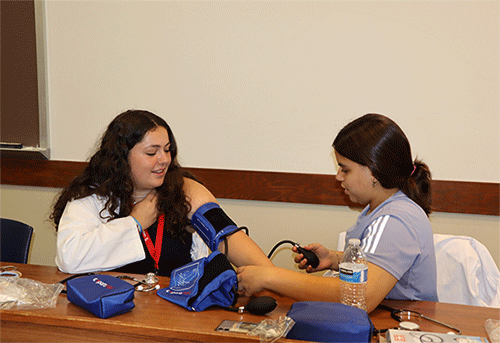
During the course of the internship, I had the invaluable opportunity to acquire fundamental clinical skills that have significantly enhanced my medical knowledge and expertise. Among the essential skills I learned were taking vital signs and conducting comprehensive neurological exams.
When it came to discussing vital signs, we delved into various methods of accurately measuring a patient’s pulse. Through hands-on practice and guidance from experienced mentors, I mastered each method, gaining the confidence to calculate heart rates in patients of all ages and conditions.
The ability to accurately take vital signs and perform neurological exams ensures that patients receive the necessary care promptly, enhancing their chances of successful treatment and recovery.

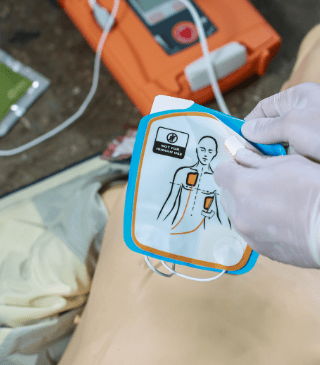
Learning cardiopulmonary resuscitation (CPR) is a vital skill that empowers individuals to respond effectively during critical life-threatening situations. CPR involves a combination of chest compressions and rescue breaths, aiming to maintain blood circulation and oxygenation in a person whose heart has stopped beating or is experiencing breathing difficulties.
By acquiring CPR training, I am equipped to provide immediate assistance to victims of cardiac arrest, drowning, or other medical emergencies, significantly increasing their chances of survival.
Moreover, learning CPR instills a sense of confidence and preparedness, enabling individuals to act promptly and decisively in times of crisis. Whether in the workplace, community settings, or at home, possessing CPR knowledge serves as a crucial link in the chain of survival and demonstrates our collective responsibility to safeguard the well-being of others in times of dire need.

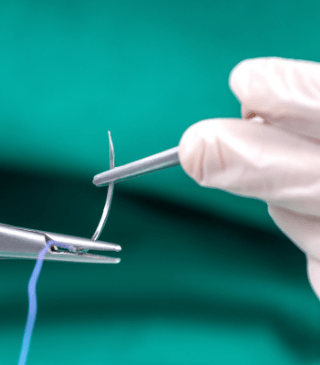
In one of the leading interactive activities of the internship, I learned and practiced multiple suturing techniques on a human-skin model. Under the expert guidance of medical professionals, I delved into the intricacies of suturing, mastering various techniques and understanding their applications in different medical scenarios.
The experience provided invaluable insights into the essential tasks performed by doctors and nurses, underscoring the significance of suturing as a fundamental skill in patient care and wound management.
As I practiced with dedication and received constructive feedback from mentors, I felt my confidence grow in handling the delicate and precise aspects of medicine.
In addition to suturing, this internship offered opportunities to explore various other medical procedures, including the application of plaster casts. These activities broadened my understanding of the multifaceted nature of medicine and illuminated the diverse skill set required in healthcare settings.